COVID -19, Is Soldiers’ Ready?
By John Swartz
Orillia Soldiers’ Memorial Hospital CEO, Carmine Stumpo, spoke with SUNonline/Orillia Thursday to answer questions regarding how prepared staff and systems are in the eventuality COVID – 19 becomes a bigger threat to the community than it already is.
There is one person, a 60-year-old man, confirmed to have the disease. He was seen at the hospital and sent home to isolate and recover. There will be more and it’s helpful to know what steps have been taken at Soldiers’ to prepare.
Stumpo mentioned several times the ability to respond depends on the community following all the recommendations to avoid getting the virus in the first place.
“There is good reason to be concerned and good reason to respond and good reason to be confident in the system if we do all the right things,” Stumpo said.
“I’m inspired and very confident that the team we have, the way the team has responded, everyone is really rising to the challenge. I do not want to diminish the challenge we see. It’s not just the hospital, it’s the entire community that needs to respond because that’s the way we are going to get through this together, if we all do our part with social distancing and flattening the curve. We cannot overemphasize this because if we are not successful in that today then I’m not sure our efforts are going to be enough. All of us need to lead by example and do our part.”
Space
We are all bracing for more cases among family and friends. All indicators in places weeks ahead of Orillia and Ontario with the progression of the virus’s world-wide conquest have seen a rise in cases requiring hospitalizations after first cases occurred. Does Soldiers’ have the capacity to deal with a large number of cases?
“We have a staged response. As things get worse we will bring more capacity online. We are looking at increasing our ICU capacity on any given day. In normal operations we have 8 ICU beds, but when you bring together all the equipment we have in operating rooms, other locations and other assistive devices for breathing, our ICU capacity could grow up to 20 beds.”
It’s not just ICU. Not everyone will need intensive care but still need to be hospitalized. Staff are planning to have space should numbers rise.
“We are looking at all of our space and seeing how to adjust capacity to serve. And that’s not just about ICU. It’s about how can we expand emergency care by overflowing (to) these different spaces. We re-think any space trying to plan out several steps ahead.”
If it gets really bad, they are looking at other facilities which might be needed.
“The scenario that the hospital is not big enough, it’s very difficult to answer that question simply because, big enough for what?” Today a testing center was opened on hospital grounds. It’s a drive-thru idea borrowed from South Korea which proved to effective. “Just by the nature of opening up the assessment center outside of the hospital we created extra capacity that helps our emergency department function better.”
“You have to look at it as what area is being overwhelmed and how do you respond. Yes, we are talking closely with City partners around spacing that could be required. We may need to move different departments around and shift them to different areas of the building.”
That doesn’t mean other facilities are ready to go right now, just that people have been looking into the what ifs.
“There’s more value in knowing how you would respond than in defining the actual response. We have a command center that meets on a daily basis, if not more frequently, to monitor what the activity is in the organization, have some solid ideas that are reasonably well developed in our back pocket.”
“We’re confident we have plans in place for the next few phases and we‘re focusing on implementing those plans. As it progresses we will address further plans going forward.”
Equipment
Much has been made in other places about ventilators being in short supply. In this area hospitals are taking a different approach.

“We do have a regional program for ventilators, but we have the capacity today of 20 assisted breathing devices in place that can be used in different ways. There also is a regional program because we want to provide them where they are needed most and we would work as a collection of hospitals to make sure the right hospitals get the devices when they need them.”
Masks, protective clothing and expendables are also a concern.
“The province has a centralized inventory. I don’t know the contents within that inventory, but there is provincial leadership to ensure there isn’t stockpiling happening at individual hospitals. They are closely monitoring these supplies. We have to recognize we are in it together as a system. It’s not one hospital or another, it’s all of us and we are trying to proceed in that way.”
“Our message to our staff is there is a global shortage of personal protective equipment and we want to make sure we have it available when we need it; no hording, use what you need, nor more, no less because that is going to be the best answer sustainably over time. What we have today does not reflect what we are going to have one week, two weeks, four weeks from now and we need to be thinking long-term.”
People
Of course, having enough medical staff and nurses is a prime consideration.
“We’ve created a central re-deployment center that tracks not only nurses availability, but skill mix, all in a staged response to know how we would redeploy.”
This week, all but the most serious procedures and surgeries were postponed. This not only frees up space, but people too.
“That capacity that’s been freed up will create beds and it will identify staff that are available to do other things. They will all be available to respond to COVID – 19.”
Already some nurses are working longer hours, people need to rest to be effective, but in crisis situation rest often doesn’t come and relief is not always available. Soldiers’ staff is thinking about having people ready to take over when needed.
“In a community like Orillia, people know who the nurses are, and the supports are and that process has been done.” He’s referring to those retired or who have left nursing for various other reasons and could be in reserve.
“We are looking at all of our part-time casual, trying to secure time and availability. We don’t know when we’ll need it, how much we will need.”
Doctors and nurses have no special immunity and the message from the top is, take yourself out of the game if you think you’ve been exposed.
“We’re leading by example on social distancing. That’s got to be the message. We’re very clear staff needs to self monitor. We’re very quick if there’s any suggested symptoms or travel history to tell people to self-isolate.”
In the end, Stumpo wants the community to know they’ve been working hard to prepare and are ready to move in whatever direction the future holds.
“I want to assure the community we are taking the appropriate view, which is our response needs to be a long-term response. We think and talk regularly about the sustainability of our actions, sustainability of how we design certain ideas.”
“Flattening the curve is all about doing actions now when you can and not waiting for the worst case scenario to materialize. However, we are being responsible in playing out that worst case scenario and making sure we are able to respond.”
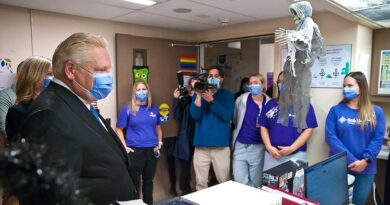
(Photo by Swartz – SUNonline/Orillia)